At the inaugural BlackDoctor.org Community Voices in Health Equity Summit, Rabin Martin Partner, Terri Jackson moderated a panel discussion on Understanding the Provider/Patient Dynamics with Compassionomics Playing a Role. She was joined by Jeana Wirtenberg, Executive Director at the Rutgers Institute for Corporate Social Innovation, Michelle Anderson-Benjamin, Metastatic Breast Cancer Survivor and Certified Mental Health Coach and Trainer, Teresa Redmond, Director, US Oncology Pan Franchise Consumer Marketing at Merck, Bryan Buckley, Director, Health Equity Initiatives at NCQA and Assistant Professor in Medicine at Georgetown University School of Medicine, and Fatima Scipion, VP, Global Patient Affairs at Blueprint Medicines.
Together, they explore the topic of Compassionomics — a topic based on the book Compassionomics: The Revolutionary Scientific Evidence that Caring Makes a Difference, where physician-scientists Stephen Trzeciak and Anthony Mazzarelli unlock compelling data revealing that compassion could be a silver bullet to improve health outcomes.
Watch the full panel presentation below & read on for Terri’s commentary:
In the following paragraphs, Terri Jackson offers her perspective and commentary on the subject:
There are distinct and meaningful differences between compassion and empathy. While both involve feelings — love, hate, sadness — compassion is characterized by actions to help the other person. Empathy is the drive of compassion; it’s the awareness, and I would venture to say, affirmation of other people’s emotional and lived experiences — an attempt to feel those same emotions from the other person’s perspective.
As the driver and precursor of compassion, empathy’s voice is encapsulated in the modern parlance of “I see you.” Empathy’s voice says, “I get you. I understand you. And I understand where you are from, where you are at, how you are feeling, and I wouldn’t want this situation to happen to me or my loved ones.” Empathy’s voice is not interpretation or hyperbole based on preconceptions drive-by racism — beliefs that we learn from sitting around the kitchen table, where we grew up, our journeys, and where we live, work, and play.
Unfortunately, our healthcare system has what I call an “empathy crisis and deficit” that is driven by medical racism. The pathway to empathy, then to compassion, is dismantling medical racism — a menace to the pathway from empathy to compassion. The American Medical Association (AMA), among other institutions such as the Centers for Disease Control and Prevention (CDC), has identified medical racism as a public health threat that is making our entire nation sick.
Here’s what medical racism can look like. One of the most quoted exemplars, for good reason, is human pain management, which is ground zero for empathy. As a practitioner, I can only imagine the human response when nuanced conversations around diabetes, CVD, CKD, PAD, cancer, pre-eclampsia, and other diseases and medical issues come into play.
A 2016 research article by PNAS found many white medical students wrongly believe Black people have a higher pain tolerance than white people. Of all the participants, 73% held at least one false belief about the biological difference between races. Examples of these beliefs include Black people having thicker skin, less sensitive nerve endings, or stronger immune systems.
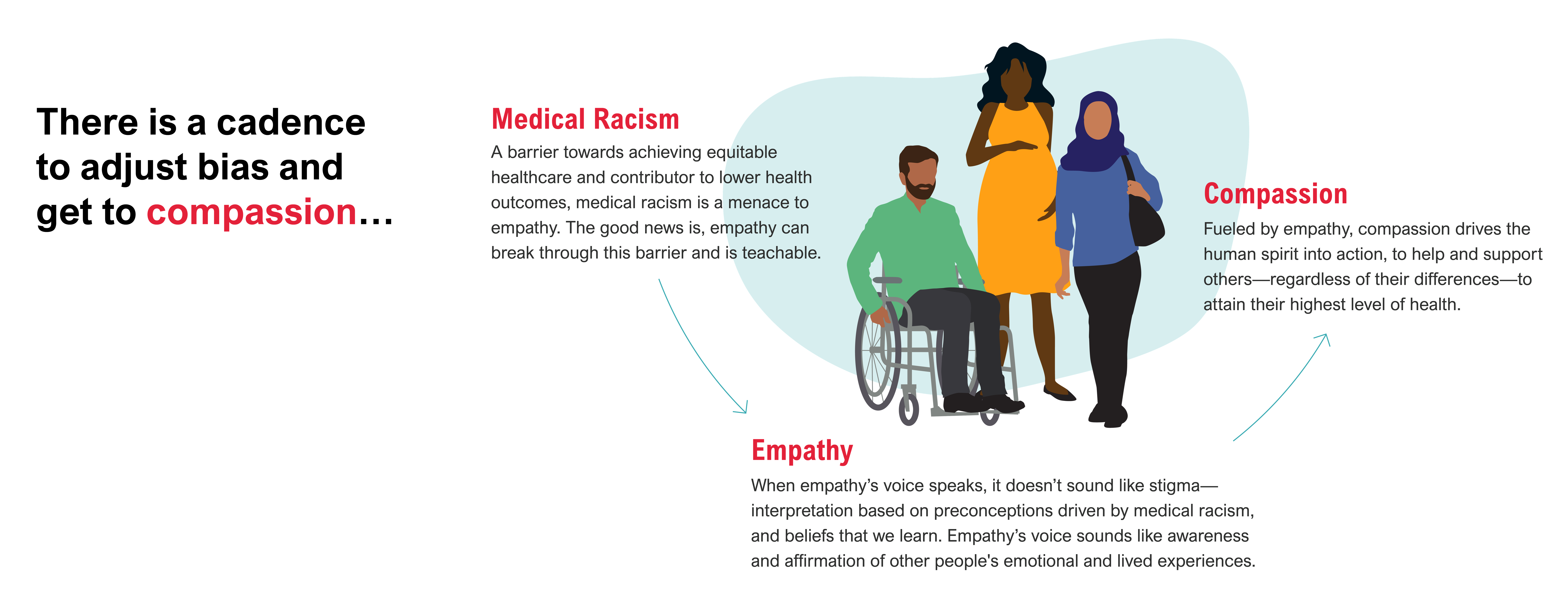
At all levels (community, healthcare point of care, etc.), we must dismantle the structures, policies, practices, and norms that assign value and determine opportunities for good health based on the way people look, or the color of their skin. Medical racism results in conditions that negatively affect the mental and physical health of millions of people, preventing them from attaining their highest level of health, and consequently, affecting the health of our nation.
The good news is that my panelists agree that empathy can be taught if we address racism in medicine. The call to action for the private sector is to invest in programs and interventions that dismantle medical racism across the value chain — from clinical trials to medicines, vaccines, and medical devices in the hands of patients.
Rabin Martin can help the private sector think through strategies and tactics to move the needle in compassionate care and treatment across the value chain — from clinical trials to medicines, vaccines, and medical devices in the hands of patietns.